What Does Protrhobin Time Test Again?
Contents
- What is prothrombin
-
- Blood coagulation procedure
- Secondary hemostasis
- Blood coagulation procedure
- Prothrombin gene mutation
- Prothrombin thrombophilia
- How is prothrombin thrombophilia inherited?
- Prothrombin thrombophilia diagnosis
- Prothrombin deficiency
- How is prothrombin deficiency inherited?
- Prothrombin thrombophilia
- What is prothrombin fourth dimension
-
- Tin can I practice prothrombin time exam at dwelling house?
- Should I have prothrombin time examination washed at the same fourth dimension of day?
- My prothrombin time results vary sometimes, nevertheless my doctor doesn't alter my prescription. Why?
- Why is my prothrombin time high?
-
- How is prothrombin time exam used?
- When is prothrombin time test ordered?
- Normal prothrombin fourth dimension
- What does the prothrombin time exam result mean?
- Fractional thromboplastin time
-
What is prothrombin
Prothrombin is a clotting factor II (clotting factor 2), which is a modular protein composed of 579 amino acids ane) . In plasma, prothrombin (clotting factor II) circulates in two forms at equilibrium, "airtight" (~80%) and "open" (~xx%), brokered by the flexibility of the linker regions ii) . In response to vascular injury, prothrombin (coagulation gene II), is converted to its active form thrombin by prothrombinase complex, a macromolecular complex composed of factor Xa (fXa), factor Va (fVa), calcium ions, and phospholipids 3) . Once in the circulation, thrombin converts fibrinogen into fibrin, activates platelets and increases endothelial permeability thereby halting the loss of blood at the site of injury 4) and facilitating vascular remodeling. Because of this critical role in biology, the prothrombin/thrombin axis remains an bonny target for anticoagulant therapy five) .
Prothrombin is synthesized past the hepatocytes in the liver as a single pre/pro-polypeptide composed of 622 amino acids half-dozen) , although elevated mRNA levels have likewise been detected in neurons and glia cells suggesting important nevertheless unexplored roles of this protein in the key nervous organisation seven) . Earlier secretion into the plasma, prothrombin undergoes extensive post-translational modifications including removal of the pre/pro peptide at the N-terminus (43 amino acids), improver of three N-glycosylations at positions 78, 100, and 373 and conversion of the get-go 10 residues of glutamic acid (Glu) to γ-carboxy glutamic acrid (Gla) eight) . The presence of glycans at position 373 increases the thermodynamic stability of the protein and confers protection to proteolysis without affecting the catalytic action of thrombin 9) . The part of the other two N-glycosylations at positions 78 and 100 remains unclear. The 10 Gla residues provide a calcium-dependent anchoring point to negatively charged phospholipid. Since prothrombin conversion to thrombin occurs on the membranes, pharmacological inhibition of the γ-carboxyl transfer reaction in the liver by vitamin K analogs, such as warfarin, represents an effective and widespread strategy to achieve profound anticoagulation in clinical practise x) . Also, mutations Glu7→ Lys in prothrombin Nijmegen and Glu29→ Gly in prothrombin Shanghai are associated with a severe bleeding disorders 11) .
The mature form of prothrombin circulates in the plasma at a concentration of 0.1 mg/ml and has a one-half-life of about 60 hours 12) . It contains four domains connected by iii intervening linkers, Lnk1 (residues 47–64), Lnk2 (residues 144–169), and Lnk3 (residues 249–284) totaling 579 amino acids (Figure 1) 13) . The Northward-terminal Gla-domain (residues one–46), named after the posttranslational modifications, is followed by two kringles, kringle-one (residues 65–143) and kringle-2 (residues 170–248), and a canonical protease domain (residues 285–579). The protease domain contains the A chain (residues 285–320) and the B chain (residues 321–579) which are connected by a conserved disulfide bail (Cys293–Cys439). The catalytic triad (His363, Asp419, and Ser525) is hosted in the B-chain and strategically located in a deep pocket surrounded past flexible loops that control access to and steer substrates toward the active site 14) .
Figure 1. Prothrombin (closed structure)
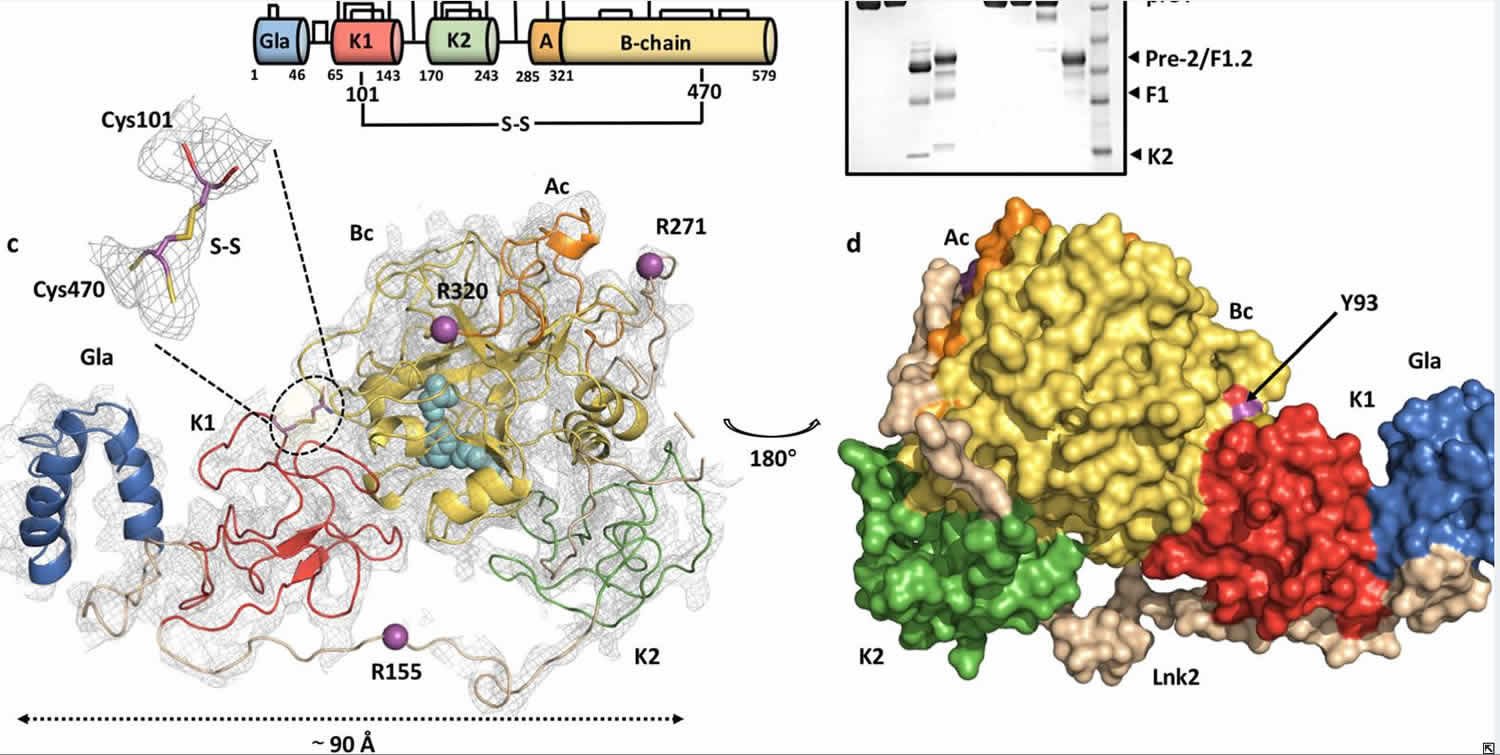
Footnote: (a) Color-coded domain architecture of prothrombin displaying the location of the engineered disulfide bond linking kringle-1 with the protease domain. Natural disulfide bonds are shown equally black lines and positioning of the cleavage sites are indicated. (b) Limited proteolysis of protWT (lanes 0–4) and proTCC (lanes 5–eight) by fXa (100 nM) in the absenteeism (−) and presence (+) of reducing agent. Shown are times 0 (lanes 1–2 and 5–6, 6 μg) and 120 min (lanes 3–four and 7–eight, ii.5 μg). The MW marker is shown in lane nine (62,49,38,28,17 kDa). The full-length gel is presented in Supplementary Fig. 5. (c) Overall construction of proTCC solved at four.1 Å resolution colored every bit in a shown as cartoon (left) or surface (correct) after 180° rotation. The key residue Tyr93 sits at the interface betwixt kringle-i and the protease domain. fXa cleavage sites Arg155, Arg271 and Arg320 are shown as spheres (magenta). The catalytic triad His363, Asp419 and Ser525 is shown as spheres (cyan). Zoom-in view of the artificial disulfide bond Cys101-Cys470. The electron density 2Fo-Fc map is countered at 1.5σ.
[Source 15) ]
Blood coagulation procedure
Blood is a necessary component of the human body, and the loss of this fluid may exist life-threatening. The human being torso protects against loss of blood through the clotting machinery. Vascular mechanisms, platelets, coagulation factors, prostaglandins, enzymes, and proteins are the contributors to the clotting mechanism which act together to form clots and finish a loss of blood 16) . Through vasoconstriction, adhesion, activation, and aggregation, the contributors class a transient plug to act as the cork to the leaking blood flow. Before long later, fibrin, the functioning form of fibrinogen, stabilizes this weak platelet plug.
The cellular components of the clotting machinery include platelets, endothelial cells, and a series of proteins, enzymes, and ions.
The clotting machinery is cleaved into two stages:
- Primary hemostasis: Formation of a weak platelet plug
- Secondary hemostasis: Stabilizing the weak platelet plug into a jell by the fibrin network
Effigy 2. Overview of blood coagulation
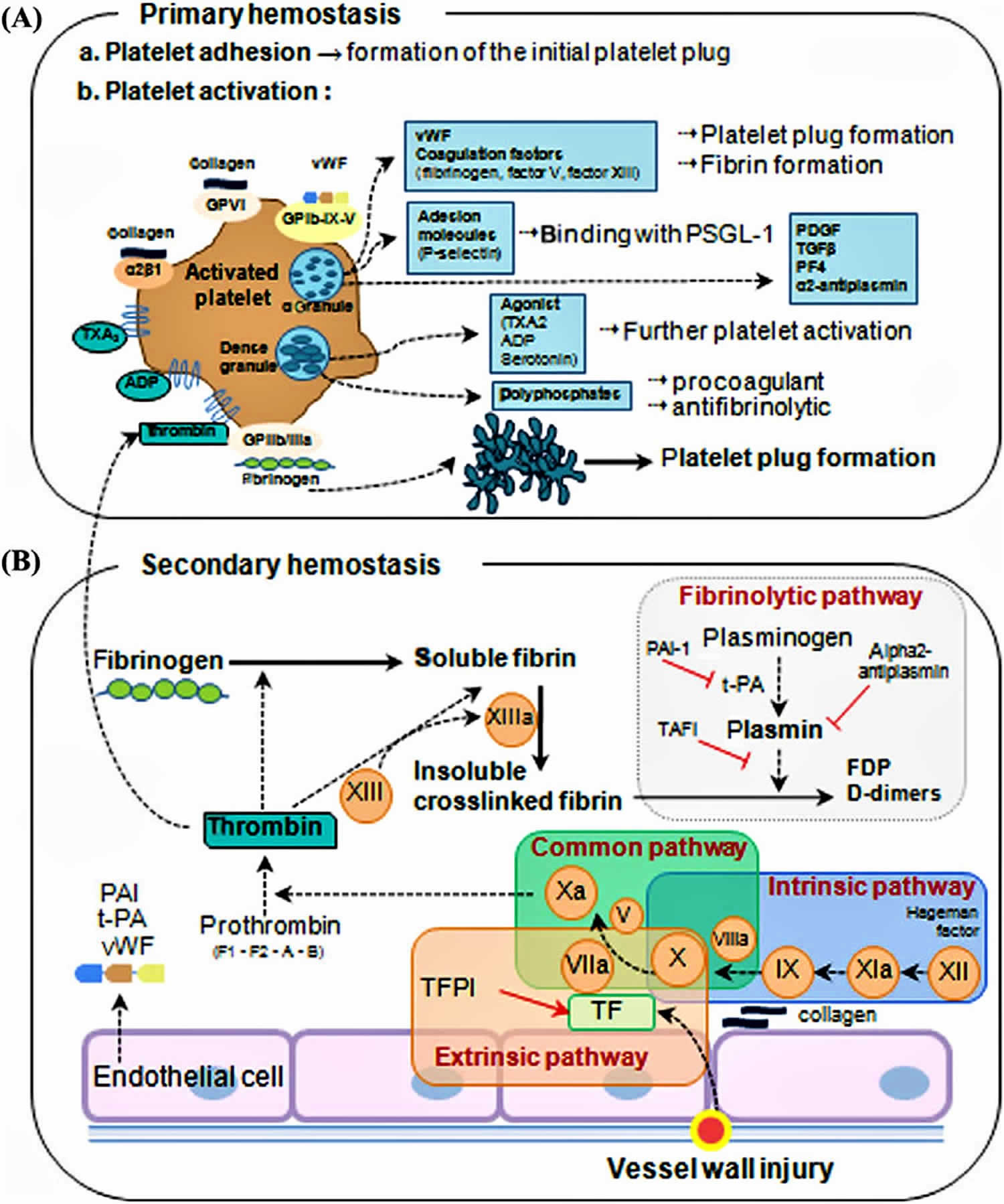
Secondary hemostasis
Secondary hemostasis involves the clotting factors interim in a cascade to ultimately stabilize the weak platelet plug. This is achieved by completing iii tasks: (i) triggering activation of clotting factors, (2) conversion of prothrombin to thrombin, and (3) conversion of fibrinogen to fibrin. These tasks are accomplished initially past one of 2 pathways; the extrinsic and intrinsic pathway, which converge at the activation of factor 10 so complete their tasks via the mutual pathway. Please annotation that calcium ions are required for the entire process of secondary hemostasis.
The extrinsic pathway includes tissue factor (TF) and factor Seven (FVII). It is initiated when tissue factor (TF) binds to factor Vii (FVII), activating FVII to factor VIIa (FVIIa), forming a TF-FVIIa complex. This complex, in turn, activates cistron X (FX). Note, the TF-FVIIa complex can also activate factor IX of the intrinsic pathway, which is called the alternating pathway. In one case Gene X is activated to FXa past TF-FVIIa circuitous, the cascade continues downward the common pathway (come across below).
The intrinsic pathway includes Hageman factor (FXII), factor I (FXI), factor IX (FIX), and factor Viii (FVIII). The process is initiated when FXII comes into contact with exposed subendothelial collagen and becomes activated to FXIIa. Subsequently, FXIIa activates FXI to FXIa, and FXIa activates Fix to FIXa. FIXa works in combination with activated factor 8 (FVIIIa) to activate factor Ten. Once Factor Ten is activated by FIXa-FVIIIa complex, the cascade continues down the common pathway (see below).
The common pathway is initiated via activation of Gene Xa. Factor Xa combines with Factor Va and calcium on phospholipid surfaces to create a prothrombinase circuitous ultimately activating prothrombin (coagulation factor II) into thrombin. This activation of thrombin occurs via serine protease cleaving of prothrombin. At present, thrombin activates gene XIIIa (FXIIIa). FXIIIa crosslinks with fibrin forming the stabilized clot.
Figure three. Coagulation pour
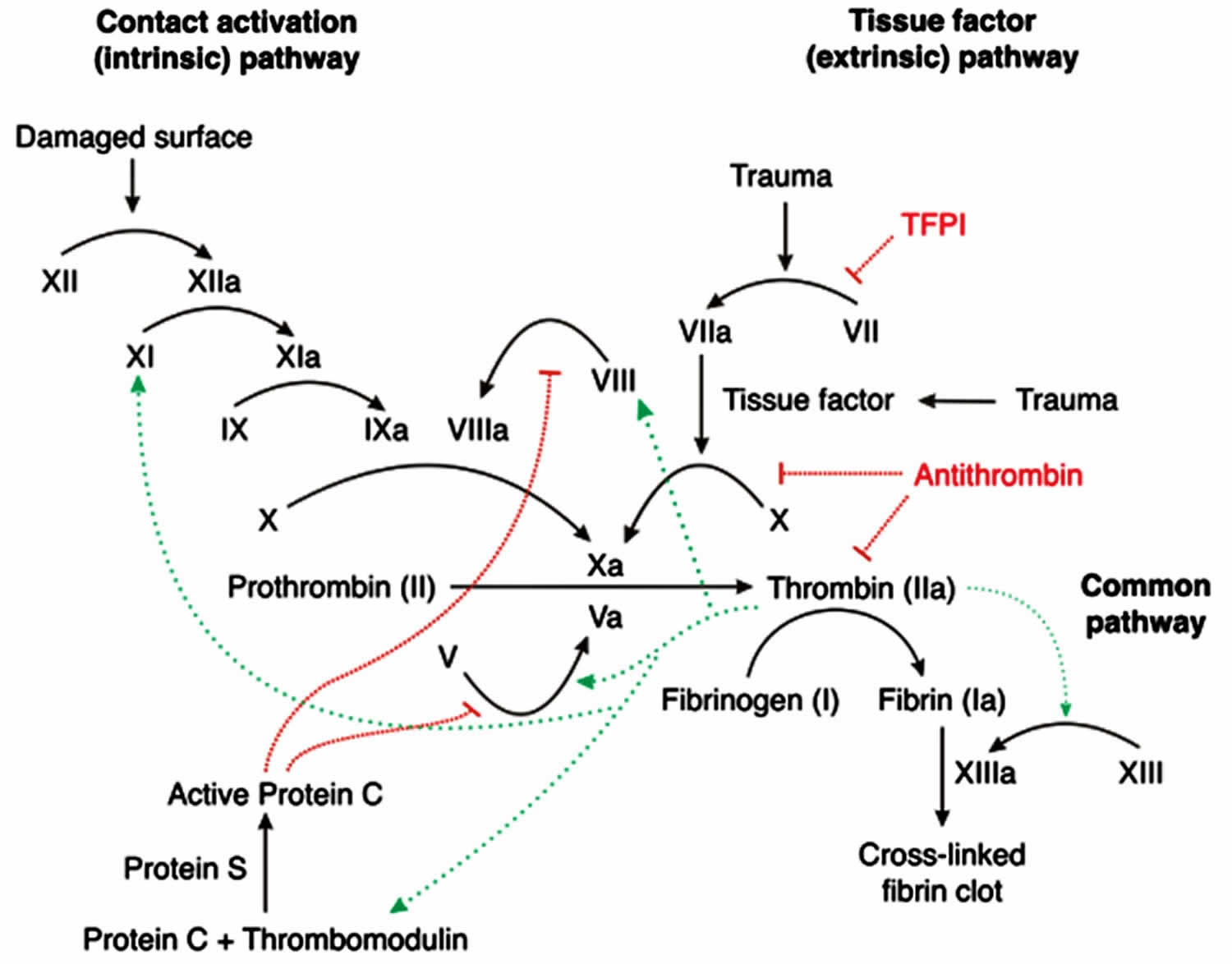
Prothrombin gene mutation
In humans, prothrombin is encoded past the F2 factor, which is located on the short arm of chromosome eleven, at position 11.ii 17) . The F2 gene contains 14 exons spanning 21 kb, and its structural integrity is critical for life. Single-nucleotide polymorphisms (SNPs) establish in patients are often associated with moderate to astringent bleeding phenotypes and the mutation G20210A in the 3′ untranslated region of the F2 factor is a well-established risk factor for prothrombin thrombophilia 18) .
Prothrombin thrombophilia
Prothrombin thrombophilia is an inherited disorder of blood clotting. Prothrombin thrombophilia is caused by a item mutation (written G20210A or 20210G>A) in the F2 cistron. People can inherit i or 2 copies of the gene mutation from their parents19) . The treatment for prothrombin thrombophilia is dependent on whether a claret clot has occurred and if there are boosted hazard factors. In individuals with a history of one or more than claret clots, blood thinning medications may be used 20) .
Thrombophilia is an increased tendency to course abnormal blood clots in blood vessels 21) . People who have prothrombin thrombophilia are at somewhat higher than average risk for a type of clot called a deep venous thrombosis, which typically occurs in the deep veins of the legs. Affected people also have an increased take a chance of developing a pulmonary embolism, which is a jell that travels through the bloodstream and lodges in the lungs. Near people with prothrombin thrombophilia never develop abnormal blood clots, however.
Prothrombin thrombophilia is the second virtually common inherited grade of thrombophilia after gene 5 Leiden thrombophilia 22) . Approximately 1 in 50 people in the white population in the Usa and Europe has prothrombin thrombophilia. This condition is less common in other ethnic groups, occurring in less than one percent of African American, Native American, or Asian populations.
Some research suggests that prothrombin thrombophilia is associated with a somewhat increased hazard of pregnancy loss (miscarriage) and may also increment the take a chance of other complications during pregnancy. These complications may include pregnancy-induced high blood pressure (preeclampsia), dull fetal growth, and early on separation of the placenta from the uterine wall (placental abruption). It is important to note, notwithstanding, that about women with prothrombin thrombophilia take normal pregnancies.
How is prothrombin thrombophilia inherited?
Prothrombin thrombophilia is inherited in an autosomal ascendant fashion 23) . This means that having 1 mutated re-create of the disease-causing gene (F2) in each prison cell may be sufficient to cause signs or symptoms of the condition. The mutation in the F2 gene that causes prothrombin thrombophilia is chosen 20210G>A (also called the 20210G>A allele). An individual tin be heterozygous (having the mutation in only i copy of the F2 gene) or homozygous (having a mutation in both copies of the F2 gene). Heterozygosity results in an increased run a risk for thrombosis; homozygosity results in more severe thrombophilia and/or increased risk for thrombosis 24) .
The risk of developing an abnormal clot in a claret vessel depends on whether a person inherits one or two copies of the F2 gene mutation that causes prothrombin thrombophilia. In the general population, the chance of developing an abnormal claret jell is nigh ane in 1,000 people per year 25) . Inheriting one copy of the F2 gene mutation increases that risk to two to 3 in 1,000 26) . People who inherit two copies of the mutation, one from each parent, may take a risk as loftier every bit 20 in 1,000 27) .
All individuals reported to date with prothrombin thrombophilia who are heterozygous for the 20210G>A allele have had an affected parent. Because of the relatively high prevalence of this allele in the general population, occasionally one parent is homozygous or both parents are heterozygous for this allele 28) .
When an private who is heterozygous for the 20210G>A allele has children, each child has a 50% (1 in 2) risk to inherit that allele and likewise be heterozygous. An individual who is homozygous will always pass one of the 20210G>A alleles to each of his/her children. If ii heterozygotes accept children together, each kid has a 25% (i in four) hazard to be homozygous (having 2 mutated copies), a 50% run a risk to be heterozygous similar each parent, and a 25% risk to inherit ii normal copies of the F2 gene.
Prothrombin thrombophilia diagnosis
No clinical signs or symptoms are specific for prothrombin thrombophilia. A confirmed diagnosis of this condition requires specific genetic testing via Dna assay of the F2 cistron, which provides instructions for making the protein prothrombin. The test identifies the presence of a common change (mutation) chosen 20210G>A29) . An individual can be a heterozygote (having one mutated copy of the F2 cistron) or a homozygote (having two mutated copies).
Virtually heterozygotes take a mildly elevated plasma concentration of prothrombin (which tin can be measured in a blood test) that is approximately 30% higher than normal. However, these values can vary profoundly, and the range of prothrombin concentrations in heterozygotes overlaps significantly with the normal range. Therefore, plasma concentration of prothrombin is not reliable for diagnosis of this condition 30) .
Individuals interested in learning more about testing for prothrombin thrombophilia should speak with a genetics professional or other healthcare provider.
Prothrombin deficiency
Prothrombin deficiency is a very rare bleeding disorder that slows the blood clotting process 31) . Prothrombin deficiency is estimated to affect 1 in 2 1000000 people in the general population 32) . People with prothrombin deficiency often feel prolonged haemorrhage following an injury, surgery, or having a tooth pulled. In severe cases of prothrombin deficiency, heavy bleeding occurs after small trauma or even in the absence of injury (spontaneous bleeding). Women with prothrombin deficiency tin accept prolonged and sometimes abnormally heavy menstrual bleeding. Serious complications tin result from bleeding into the joints, muscles, brain, or other internal organs. Milder forms of prothrombin deficiency practise not involve spontaneous bleeding, and the condition may only go apparent following surgery or a serious injury.
Prothrombin deficiency is caused past changes (mutations) in the F2 cistron 33) . In that location are two types of inherited prothrombin deficiency. Type I or hypoprothrombinemia and type II or dysprothrombinemia. Inheritance of both types is autosomal recessive 34) . Blazon I or hypoprothrombinemia is more severe, and it is characterized by a decreased level of commonly functioning poly peptide, and therefore, by a decrease in proteinactivity. Type II or dysprothrombinemia is characterized by normal or low-normal levels of an abnormal (dysfunctional) poly peptide. Bleeding symptoms vary depending on the amount of residual functional activeness 35) .
In other cases, prothrombin deficiency is acquired. This ways that prothrombin deficiency develops afterwards in life and is not caused by a genetic change. Potential causes of acquired prothrombin deficiency include astringent liver disease, vitamin K deficiency, or an autoimmune response that prevents the prothrombin protein from working properly 36) .
Diagnosis is based on laboratory test results that are consistent with the prothrombin deficiency.
The handling of prothrombin deficiency depends on the exact crusade and severity of the disease. When a person with prothrombin (gene Ii) deficiency has bleeding episodes, fresh frozen plasma, the function of the blood that contains the blood clotting factors, tin can be used to treat the bleeding. If a person with prothrombin deficiency requires surgery, plasma substitution therapy may be used to increment factor II (prothrombin) levels prior to surgery. People who have acquired prothrombin deficiency may benefit from taking vitamin K. Some people with prothrombin deficiency may be recommended to avoid activities that can result in physical contact or injuries 37) . In some cases, prothrombin circuitous concentrates can be used to increment factor II levels. However, because these concentrates contain clotting factors other than factor II, they can outcome in an increased risk for blood to clot too quickly within the blood vessels (thromboembolic outcome) 38)
A grade of the disease that is not inherited (caused) can be caused by vitamin K deficiency, liver disease, or an autoimmune response. The underlying cause of acquired prothrombin deficiency should exist treated in social club to relieve symptoms of the affliction 39) .
How is prothrombin deficiency inherited?
Prothrombin deficiency is inherited in an autosomal recessive pattern, which means both copies of the gene in each cell have mutations. The parents of an individual with an autosomal recessive condition each deport one copy of the mutated gene, only they typically do not prove signs and symptoms of the condition.
What is prothrombin time
Prothrombin time (PT) is a blood exam that measures the time it takes for the liquid portion (plasma) of your blood to clot. The prothrombin time is a test that helps evaluate a person's ability to appropriately form blood clots. The international normalized ratio (INR) is a calculation based on results of a prothrombin fourth dimension that is used to monitor individuals who are being treated with the blood-thinning medication (anticoagulant) warfarin (Coumadin®). A related blood examination is fractional thromboplastin time (PTT).
A prothrombin fourth dimension measures the number of seconds it takes for a clot to grade in a person's sample of blood after substances (reagents) are added. The prothrombin time is often performed with a fractional thromboplastin time (PTT) and together they assess the amount and part of proteins called coagulation factors that are an important role of proper claret clot formation.
In your body, when there is an injury and haemorrhage occurs, the clotting process called hemostasis begins. This procedure involves in part a serial of sequential chemical reactions chosen the coagulation pour, in which coagulation or "clotting" factors are activated one after another and result in the formation of a clot. There must exist a sufficient quantity of each coagulation cistron, and each must part properly, in gild for normal clotting to occur. Also trivial can lead to excessive haemorrhage; too much may pb to excessive clotting.
In a test tube during a laboratory exam, in that location are two "pathways" that tin can initiate clotting, the then-chosen extrinsic and intrinsic pathways. Both of these then merge into a mutual pathway to complete the clotting process. The prothrombin fourth dimension test evaluates how well all of the coagulation factors in the extrinsic and common pathways of the coagulation cascade work together. Included are: factors I (Fibrinogen), II (Prothrombin), V, VII and Ten. The PTT examination evaluates those protein factors that are part of the intrinsic and common pathways: XII, XI, 9, VIII, X, V, 2 (prothrombin), and I (fibrinogen) as well every bit prekallikrein (PK) and high molecular weight kininogen (HK). The prothrombin time and PTT evaluate the overall ability to produce a clot in a reasonable amount of time and, if any of these factors are deficient in quantity or not functioning properly, the test results will be prolonged.
The prothrombin time test is commonly measured in seconds and is compared to a normal range that reflects prothrombin time values in healthy individuals. Considering the reagents used to perform the prothrombin time test vary from 1 laboratory to some other and fifty-fifty within the same laboratory over time, the normal ranges also will fluctuate. To standardize results across different laboratories in the U.S. and the world, a World Health Organization (WHO) committee developed and recommended the apply of the Internationalized Normalized Ratio (INR), calculated based on the prothrombin time examination effect, for people who are receiving the anticoagulant warfarin (Coumadin®).
The INR (Internationalized Normalized Ratio) is a adding that adjusts for changes in the prothrombin fourth dimension reagents and allows for results from different laboratories to be compared. Nearly laboratories report both prothrombin time and INR values whenever a prothrombin time test is performed. The INR should be simply applicable, however, for those taking the blood-thinning medication warfarin.
Tin can I do prothrombin fourth dimension examination at home?
Aye, if you will be taking warfarin for an extended period of time. The Food and Drug Administration has canonical several home prothrombin fourth dimension and international normalized ratio (INR) testing systems. However, habitation testing is usually done in the context of a home-based coagulation management program that involves patient training and defined response and management protocols.
Should I have prothrombin time test done at the aforementioned time of mean solar day?
It is not generally necessary to have your prothrombin fourth dimension and international normalized ratio (INR) measured at a particular time of twenty-four hours. It is, however, important that you take your warfarin medication at the same time each day to maintain a continuous level. If your healthcare provider increases or decreases your dosage, he or she may want yous to take your claret rechecked in a couple of days or so to judge the effect of the dosage modify on your prothrombin time/INR (it is not an firsthand issue).
My prothrombin time results vary sometimes, yet my doctor doesn't change my prescription. Why?
Affliction, change in diet, and some medications (every bit mentioned to a higher place) can alter prothrombin fourth dimension results. Certain foods, such every bit beefiness and pork liver, light-green tea, broccoli, chickpeas, kale, turnip greens, and soybean products contain large amounts of vitamin 1000 and tin alter prothrombin fourth dimension results. The blood collection technique and the difficulty in obtaining the claret sample tin also affect test results. If your healthcare provider has concerns about the stability of your prothrombin time/INR, he or she may examination your claret more frequently.
Why is my prothrombin fourth dimension high?
Prothrombin time (PT) may be prolonged due to deficiencies of factors X, Vii, Five, and Ii of the extrinsic pathway, presence of inhibitors, or oral anticoagulation therapy.
Prothrombin time (PT) is not useful for detecting deficiencies of coagulation factors that accept no influence on the prothrombin time exam (eg, factors Viii, IX, Xi, XII, 13).
How is prothrombin fourth dimension test used?
The prothrombin time (PT) is used, often along with a partial thromboplastin time (partial thromboplastin time), to aid diagnose the cause of unexplained bleeding or inappropriate blood clots. The international normalized ratio (INR) is a calculation based on results of a prothrombin time and is used to monitor individuals who are being treated with the blood-thinning medication (anticoagulant) warfarin (Coumadin®).
Several proteins chosen coagulation factors are involved in the process that the trunk uses to form blood clots to help stop bleeding (hemostasis). When an injury occurs and bleeding begins, some coagulation factors are activated in a sequence of steps (coagulation cascade) that eventually help to form a clot. There must be a sufficient quantity of each coagulation gene, and each must function properly, in club for normal clotting to occur. Too piffling can lead to excessive bleeding; too much may lead to excessive clotting.
The prothrombin fourth dimension and INR (Internationalized Normalized Ratio) are used to monitor the effectiveness of the anticoagulant warfarin. This drug affects the role of the coagulation cascade and helps inhibit the germination of claret clots. It is prescribed on a long-term basis to people who have experienced recurrent inappropriate blood clotting. The goal of warfarin therapy is to maintain a residual between preventing clots and causing excessive bleeding. This balance requires conscientious monitoring. The INR (Internationalized Normalized Ratio) can exist used to adapt a person's drug dosage to become the PT into the desired range that is right for the person and his or her condition.
Warfarin may be prescribed for conditions such equally:
- Irregular heartbeat (atrial fibrillation)
- The presence of artificial heart valves
- Deep vein thrombosis (DVT), pulmonary embolism (PE)
- Antiphospholipid syndrome
- Occasionally, in heart attacks with certain risk factors
The prothrombin time test may be used along with a partial thromboplastin time (PTT) as the starting points for investigating excessive bleeding or clotting disorders. The prothrombin time evaluates the coagulation factors VII, X, V, II and I (fibrinogen). The fractional thromboplastin fourth dimension (PTT) test evaluates coagulation factors XII, XI, IX, 8, X, V, II (prothrombin), and I (fibrinogen) as well as prekallikrein (PK) and high molecular weight kininogen (HK). By evaluating the results of the prothrombin time and fractional thromboplastin time together, a wellness practitioner can proceeds clues every bit to what bleeding or clotting disorder may be present. These tests are not diagnostic by themselves but ordinarily provide data on whether further tests may be needed.
Examples of other testing that may be done along with a prothrombin time and partial thromboplastin fourth dimension or in follow up to abnormal results include:
- Platelet count – to determine if platelets are decreased, which can cause excessive bleeding
- Thrombin time testing – sometimes ordered to help rule out a fibrinogen aberration
- Fibrinogen testing – may be done to rule out a low level or dysfunction of fibrinogen as a cause of a prolonged PT
- Coagulation cistron tests – these mensurate the activity (office) of coagulation factors. They tin can observe reduced levels of the protein or proteins that don't work properly (take reduced part). Rarely, the antigen level (quantity) of a coagulation cistron may also be measured.
- von Willebrand factor – sometimes ordered to help make up one's mind if von Willebrand illness is the cause of a prolonged partial thromboplastin fourth dimension
Based on carefully obtained patient histories, the partial thromboplastin time and prothrombin time tests are sometimes selectively performed equally pre-surgical or before other invasive procedures to screen for potential bleeding tendencies.
When is prothrombin time test ordered?
A prothrombin time and INR are ordered on a regular basis when a person is taking the anticoagulant drug warfarin to ensure that the prescription is working properly and that the prothrombin time/INR is appropriately prolonged. There is no set frequency for doing the test. A health practitioner will lodge them often enough to make sure that the drug is producing the desired issue – that information technology is increasing the person'south clotting fourth dimension to a therapeutic level without significant chance of excessive bleeding or bruising.
The prothrombin fourth dimension may be ordered when a person who is not taking anticoagulant drugs has signs or symptoms of excessive bleeding or clotting, such as:
- Unexplained bleeding or easy bruising
- Nosebleeds
- Bleeding gums
- A blood clot in a vein or artery
- An astute condition such as disseminated intravascular coagulation (DIC) that may cause both haemorrhage and clotting as coagulation factors are used upwards at a rapid rate
- A chronic condition such as severe liver disease that may affect hemostasis
Prothrombin fourth dimension, along with fractional thromboplastin time (PTT), may be ordered prior to surgery when the surgery carries an increased take a chance of blood loss and/or when the person has a clinical history of bleeding, such every bit frequent or excessive nosebleeds and easy bruising, which may indicate the presence of a haemorrhage disorder.
Normal prothrombin time
Prothrombin fourth dimension is measured in seconds. Near of the time, results are given equally what is called INR (international normalized ratio).
If y'all are not taking blood thinning medicines, such as warfarin, the normal range for your prothrombin time results is:
- 11 to 13.5 seconds
- INR of 0.8 to i.1
If you are taking warfarin to prevent blood clots, your provider volition nearly likely choose to keep your INR between 2.0 and 3.0.
Ask your doctor what outcome is right for y'all.
Normal value ranges may vary slightly among different laboratories. Some labs utilize different measurements or examination unlike samples. Talk to your doc about the significant of your specific test results.
Some consumed substances, such as alcohol, can affect the prothrombin fourth dimension and INR tests. Some antibiotics tin increase the prothrombin fourth dimension and INR. Barbiturates, oral contraceptives and hormone-replacement therapy (HRT), and vitamin K (either in a multivitamin or liquid nutrition supplement) may subtract prothrombin time. Certain foods, such as beefiness and pork liver, greenish tea, broccoli, chickpeas, kale, turnip greens, and soybean products, contain large amounts of vitamin Grand and can change prothrombin time results. It is of import that a healthcare provider know about all of the drugs, supplements, and foods that a person has ingested recently and then that the prothrombin fourth dimension and INR results are interpreted and used correctly.
Some laboratories will report a prothrombin time as a percentage of normal, although this is not a common practice.
What does the prothrombin time exam result hateful?
For people taking warfarin, most laboratories report prothrombin time results that have been adjusted to the INR. These people should have an INR of 2.0 to iii.0 for bones "blood-thinning" needs. For some who accept a high risk of a blood clot, the INR needs to exist higher – virtually 2.5 to 3.v.
The exam result for a prothrombin time depends on the method used, with results measured in seconds and compared to the normal range established and maintained by the laboratory that performs the test. This normal range represents an boilerplate value of salubrious people who live in that area and will vary somewhat from lab to lab. Someone who is not taking warfarin would compare their prothrombin fourth dimension test result to the normal range provided with the test result by the laboratory performing the exam.
A prolonged prothrombin time ways that the blood is taking too long to form a clot. This may exist caused by atmospheric condition such equally liver illness, vitamin Grand deficiency, or a coagulation gene deficiency. The prothrombin time result is often interpreted with that of the partial thromboplastin time (PTT) in determining what condition may be present.
If y'all are not taking blood thinning medicines, such as warfarin, an INR result to a higher place 1.one means your blood is clotting more slowly than normal. This may be due to:
- Bleeding disorders, a grouping of weather condition in which there is a problem with the body'due south claret clotting process.
- Disorder in which the proteins that control claret clotting get over active (disseminated intravascular coagulation).
- Liver disease.
- Low level of vitamin K.
If you are taking warfarin to foreclose clots, your provider will most likely choose to keep your INR between 2.0 and 3.0:
- Depending on why y'all are taking the blood thinner, the desired level may be different.
- Even when your INR stays between ii.0 and 3.0, you are more likely to take haemorrhage problems.
- INR results higher than 3.0 may put you at even college risk for bleeding.
- INR results lower than two.0 may put you at risk for developing a claret clot.
INR therapeutic ranges for orally administered drugs:
- Standard-intensity warfarin therapeutic range: ii.0 to 3.0
- Loftier-intensity warfarin therapeutic range: ii.5 to 3.5
Note: The INR should just exist used for patients on stable oral anticoagulant therapy, though it is reported for all patients despite whether they are receiving oral anticoagulants.
A prothrombin time result that is as well loftier or too low in someone who is taking warfarin (Coumadin) may be due to:
- The wrong dose of medicine
- Drinking alcohol
- Taking certain over-the-counter (OTC) medicines, vitamins, supplements, common cold medicines, antibiotics, or other medicines
- Eating food that changes the style the blood-thinning medicine works in your body
Your provider will teach you about taking warfarin (Coumadin) the proper way.
Table i. Estimation of prothrombin time (PT) and partial thromboplastin time (PTT) in patients with a bleeding or clotting syndrome
| Prothrombin time (PT) result | Partial Thromboplastin Fourth dimension (PTT) event | Examples of conditions that may be present |
|---|---|---|
| Prolonged | Normal | Liver disease, decreased vitamin Thou, decreased or defective factor Vii, chronic depression-grade disseminated intravascular coagulation (DIC), anticoagulation drug (warfarin) therapy |
| Normal | Prolonged | Decreased or defective factor VIII, Ix, Xi, or XII, von Willebrand disease (astringent type), presence of lupus anticoagulant, autoantibody confronting a specific factor (east.k., cistron 8) |
| Prolonged | Prolonged | Decreased or defective factor I, II, V or X, severe liver disease, acute DIC, warfarin overdose |
| Normal | Normal or slightly prolonged | May indicate normal hemostasis; however, PT and PTT tin be normal in atmospheric condition such as mild deficiencies in coagulation factor(s) and mild form of von Willebrand disease. Further testing may be required to diagnose these conditions. |
Partial thromboplastin fourth dimension
The fractional thromboplastin fourth dimension (PTT) is a screening test that helps evaluate a person'south ability to appropriately form claret clots. It measures the number of seconds information technology takes for a clot to course in a person's sample of blood after substances (reagents) are added. The partial thromboplastin time assesses the amount and the function of certain proteins called coagulation factors that are an important office of claret clot germination.
The partial thromboplastin time is used to evaluate the coagulation factors XII, XI, 9, Eight, X, V, Ii (prothrombin), and I (fibrinogen) too as prekallikrein (PK) and loftier molecular weight kininogen (HK). A PT test evaluates the coagulation factors Vii, Ten, Five, Ii, and I (fibrinogen). Past evaluating the results of the two tests together, a health practitioner can gain clues every bit to what bleeding or clotting disorder may be nowadays. The partial thromboplastin time and PT are not diagnostic merely unremarkably provide information on whether further tests may be needed.
Some examples of uses of a fractional thromboplastin fourth dimension (PTT) include:
- To identify coagulation factor deficiency; if the fractional thromboplastin time is prolonged, further studies can then exist performed to identify what coagulation factors may exist deficient or dysfunctional, or to determine if an antibody to a coagulation factor (a specific inhibitor) is present in the blood.
- To detect nonspecific autoantibodies, such as lupus anticoagulant; these are associated with clotting episodes and with recurrent miscarriages. For this reason, fractional thromboplastin fourth dimension testing may be performed as role of a clotting disorder panel to assistance investigate recurrent miscarriages or diagnose antiphospholipid syndrome (APS). A variation of the fractional thromboplastin time chosen the LA-sensitive fractional thromboplastin time may be used for this purpose.
- To monitor standard (unfractionated, UF) heparin anticoagulant therapy; heparin is an anticoagulation drug that is given intravenously (Four) or past injection to prevent and to treat blood clots (embolism and thromboembolism). Information technology prolongs partial thromboplastin time. When heparin is administered for therapeutic purposes, it must be closely monitored. If also much is given, the treated person may bleed excessively; with too little, the treated person may keep to clot.
- Based on carefully obtained patient histories, the fractional thromboplastin time (PTT) and prothrombin fourth dimension (PT) tests are sometimes selectively performed as pre-surgical or earlier other invasive procedures to screen for potential haemorrhage tendencies.
Examples of other testing that may be done along with a fractional thromboplastin fourth dimension (PTT) or in follow upward to abnormal results include:
- Platelet count – should always exist monitored during heparin therapy to promptly find any heparin-induced thrombocytopenia
- Thrombin fourth dimension testing – sometimes ordered to help rule out heparin contamination
- Fibrinogen testing – may be done to rule out a low level of fibrinogen as a crusade of a prolonged partial thromboplastin fourth dimension
- When an initial partial thromboplastin time is prolonged, a second partial thromboplastin time test is performed by mixing the person's plasma with pooled normal plasma (a collection of plasma from a number of normal donors). If the partial thromboplastin time time returns to normal ("corrects"), it suggests a deficiency of ane or more of the coagulation factors in the person's plasma. If the time remains prolonged, then the problem may be due to the presence of an aberrant specific factor inhibitor (autoantibody) or nonspecific lupus anticoagulant.
- Coagulation cistron tests – these measure the action (function) of coagulation factors. They tin can detect reduced levels of the protein or proteins that don't work properly (have reduced role). Rarely, the antigen level (quantity) of a coagulation factor may also be measured.
- Dilute Russell viper venom examination (DRVVT) – a test that may be done if the presence of lupus anticoagulant is suspected.
- von Willebrand factor – sometimes ordered to assist determine if von Willebrand affliction is the crusade of a prolonged partial thromboplastin time
When torso tissue(s) or blood vessel walls are injured, haemorrhage occurs and a procedure chosen hemostasis begins. Pocket-size cell fragments called platelets adhere to and so clump (amass) at the injury site. At the aforementioned time, a process called the coagulation cascade begins and coagulation factors are activated. Through the cascading reactions, threads chosen fibrin form and crosslink into a net that adheres to the injury site and stabilizes it. Forth with the platelets adhering, this forms a stable blood clot to seal off injuries to blood vessels, prevents boosted blood loss, and gives the damaged areas time to heal.
Each component of this hemostatic process must function properly and exist present in sufficient quantity for normal blood clot formation. If at that place is a deficiency in one or more of these factors, or if the factors role abnormally, then a stable jell may non course and haemorrhage continues.
With a partial thromboplastin time, a person'south sample is compared to a normal reference interval for clotting time. When a person's partial thromboplastin time takes longer than normal to clot, the partial thromboplastin fourth dimension is considered "prolonged." A prolonged fractional thromboplastin time may be due to a status that decreases or creates a dysfunction in one or more coagulation factors. Less often, it may be due to a condition in which the body produces certain antibodies directed against one or more coagulation factors, affecting their function.
Sometimes a partial thromboplastin time may be prolonged because the person tested produces an autoantibody called an antiphospholipid antibody that interferes with the exam. This type of antibiotic affects the results of the test because information technology targets substances chosen phospholipids that are used in the partial thromboplastin time. Though antiphospholipid antibodies tin prolong the fractional thromboplastin time test consequence, in the body they are associated with excessive clotting. A person who produces these antibodies may be at an increased hazard for a blood clot. A fractional thromboplastin time perchance used equally part of an evaluation of a person with signs and symptoms of excessive clotting or antiphospholipid syndrome. (Meet the article on Antiphospholipid Antibodies for additional details.)
When a partial thromboplastin time is used to investigate bleeding or clotting episodes, it is often ordered along with a prothrombin fourth dimension (PT). A wellness practitioner volition evaluate the results of both tests to help make up one's mind the cause of haemorrhage or clotting episode(due south).
It is now understood that coagulation tests such equally the prothrombin time and partial thromboplastin time are based on what happens artificially in the test setting (in vitro) and thus practise not necessarily reflect what really happens in the body (in vivo). Even so, they can exist used to evaluate certain components of the hemostasis system. The partial thromboplastin time and prothrombin time tests each evaluate coagulation factors that are part of different groups of chemical reaction pathways in the cascade, called the intrinsic, extrinsic, and common pathways.
References [ + ]
Source: https://healthjade.com/prothrombin/
0 Response to "What Does Protrhobin Time Test Again?"
Post a Comment